Heart disease is any number of conditions where plaque builds up in the heart’s vessels and arteries, putting a lot of stress on the heart muscle to keep pumping blood. (Learn More, Heart Disease and Plaque)
Some of the risk factors are genetic (age and family history), while some are based on lifestyle (poor diet, not enough exercise, and unhealthy habits). (Learn More, Risk Factors)
Symptoms of heart disease are mostly determined by the cause and nature of the form of heart disease, but they largely involve breathing difficulty, lack of stamina, and other problems because of insufficient blood flow in the body. (Learn More, Heart Disease Symptoms)
Effective treatment for heart disease involves early diagnosis, followed by medication and lifestyle changes to complement the type of heart disease that is at play. (Learn More, Finding Effective Treatments for Heart Disease)
What Is Heart Disease?
The term heart disease, explains Mayo Clinic, refers to a number of different conditions that affect the functioning and health of the heart. Such conditions include coronary artery disease (an example of a blood vessel disease), problems with heart rhythm, and congenital heart defects (heart problems that people are born with).
There are many other types of heart disease, some based on genetics, some based on lifestyle, and others based on related medical conditions. Most of these can be treated or even prevented with exercise, good diet, not smoking, and other sound lifestyle choices. Others might require medications and, in serious circumstances, surgery.
Heart Disease and Plaque
Heart disease is the condition of plaque developing in the blood vessels and arteries that lead to the heart. Plaque is a yellowish, waxy buildup of minerals, fatty molecules, and cholesterol. It builds up over time when the inner lining of an artery is damaged, either as the result of high cholesterol, triglycerides, high blood pressure, or cigarette smoking.
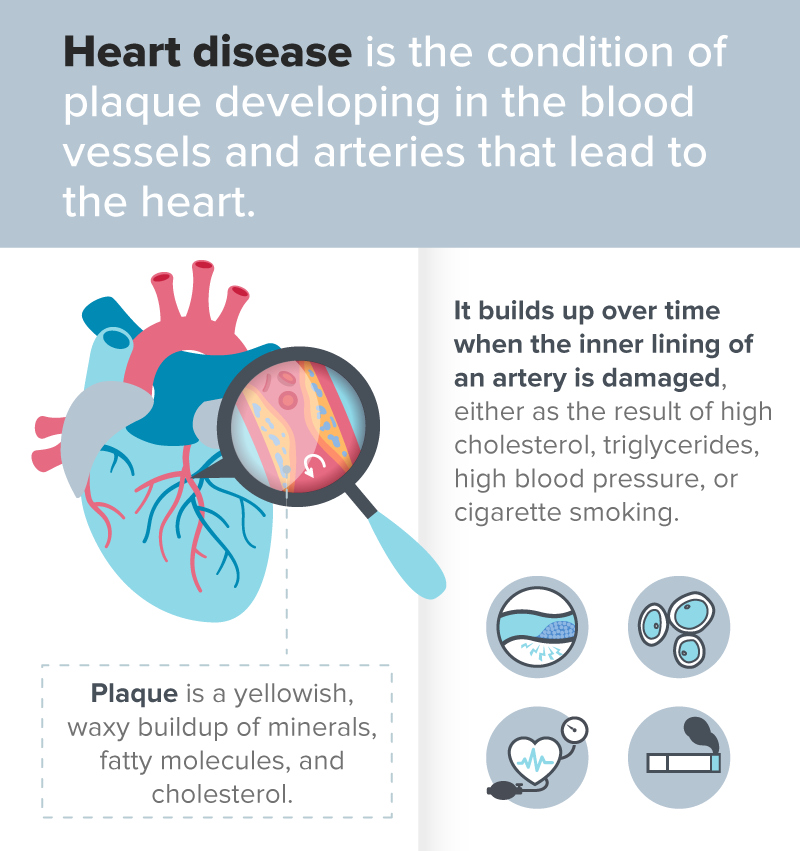
The accumulation of the plaque stops oxygen and vital nutrients from reaching the heart. Blood will also clot inside an affected artery.
Risk Factors
Heart disease has a number of risk factors that determine the likelihood of its development. Some of them, like age and genetics are inevitable. Women over the age of 55 and men over the age of 45 have a higher risk for developing heart disease. People who have close family members with heart disease are at a higher risk of getting it themselves.
Many of the other risk factors, however, can be acted upon. They include the following:
- High cholesterol and blood pressure
- Obesity
- Diabetes
- Not getting enough exercise
- Smoking
- Bad diet (high in fat proteins, sugar, sodium, and trans fats)
- Certain mental health conditions, like major depression or chronic stress
Heart Disease Symptoms
The symptoms of heart disease differ based on the nature of the specific form of heart disease.
Heart disease is the result of blockage in the blood vessels (known specifically as atherosclerotic disease). It strikes men and women differently. Men will experience chest pain more than women, while women will struggle with fatigue, nausea, and difficulty breathing as well as some general discomfort in the chest (angina).
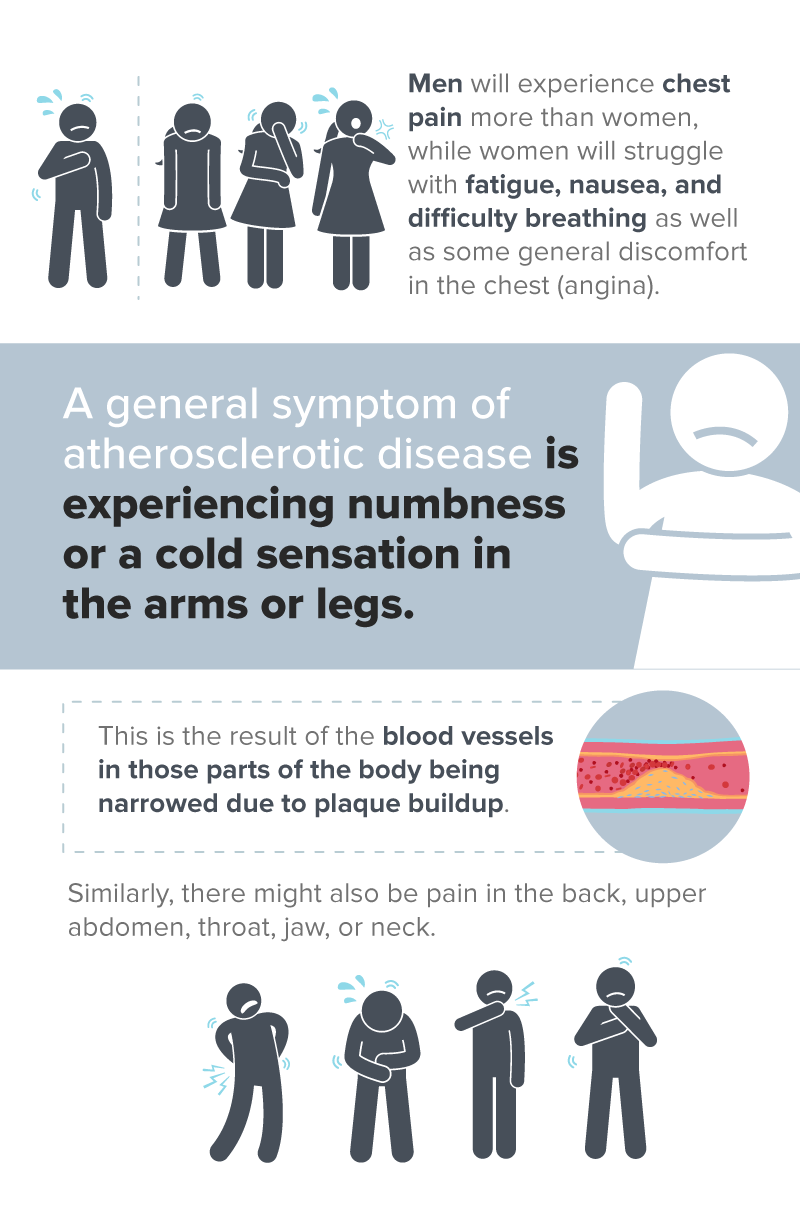
A general symptom of atherosclerotic disease is experiencing numbness or a cold sensation in the arms or legs. This is the result of the blood vessels in those parts of the body being narrowed due to plaque buildup. Similarly, there might also be a pain in the back, upper abdomen, throat, jaw, or neck.
Regular testing can determine the risk of cardiovascular disease, but a diagnosis might not be given until a patient suffers a heart attack, stroke, or heart failure. People who fit the profile for this kind of heart attack (based on age, genetics, gender, lifestyle, and other health concerns) should be on the lookout for the symptoms mentioned above.
Heart Arrhythmias and Congenital Defects
Heart disease that is the result of abnormal heartbeats (heart arrhythmias, where the heart beats too slowly, too quickly, or simply without a consistent pattern) can lead to its own symptoms.
- Dizziness
- Difficulty breathing
- Fainting
Congenital heart defects are ones that people are born with. They are usually detected shortly after birth. Children born with these defects might display the following:
- Cyanosis (skin that is pale gray or blue)
- Swelling around the eyes, abdomen, or legs
- Shortness of breath during breastfeeding and poor weight gain
There are other symptoms of congenital heart defects (quickly running out of breath during exercise, low stamina levels, or swelling in the ankles and feet), but these are not typically diagnosed until much later in childhood or even into adulthood. These symptoms are not considered life-threatening.
Dilated Cardiomyopathy and Endocarditis
Another cause of heart disease is having a weak heart muscle, a condition known as dilated cardiomyopathy. In the early stages of this form of heart disease, there may be no evident symptoms; however, as the condition progresses, it will show itself in these symptoms:
- Losing breath easily, whether at rest or during activity
- Swelling in the ankles and the feet
- Fatigue
- Dizziness, lightheadedness, and fainting spells
- Heartbeats that feel too light, too strong, or irregular
Certain other health problems can infect the heart, which causes its own set of heart disease symptoms. Endocarditis, for example, is an infection that targets the endocardium, which is the inner membrane that separates the valves and chambers of the heart.
Symptoms of endocarditis, and other similar heart infections, include the following:
- Fever
- Swelling in the abdomen and legs
- Dry cough
- Unstable heartbeat pattern
- Shortness of breath
- Fatigue
- Rashes
Valvular Heart Disease
There are four valves in the heart: tricuspid, pulmonary, mitral, and aortic valve. Their function is to control the direct flow of blood to the heart by working in unison to open and close.
There are a number of conditions that can damage the valves, either narrowing them (stenosis), causing them to leak (insufficiency or regurgitation), or causing them to not close properly (prolapse).
Valvular heart disease is the condition of one or more of the four valves not working properly. Depending on which valve is affected, the symptoms will be slightly different. Broadly speaking, patients experiencing valvular heart disease will experience fatigue, problems with their heartbeat, pain in the chest, fainting, and breathing difficulties.
It is vital that a patient call a doctor or 911 if they experience any of these symptoms. Time is of the essence when a heart disease symptom acts up. Heart disease is much easier to treat when acted upon early, so a patient having any of the risk factors for heart disease should talk with their doctor as soon as possible.
Finding Effective Treatments for Heart Disease

Some ways to treat heart disease or even prevent it include managing body weight, getting regular exercise, adopting a diet that focuses on the health of the heart, and certain other lifestyle changes.
In terms of body weight, it is recommended by the National Institute of Diabetes and Digestive and Kidney Disorders that a person loses between 5 and 10 percent of their body weight. This will lower the chances of them developing cardiovascular disease.
In terms of exercise, around 150 minutes of moderate or intense physical activity every week is recommended by the American Heart Association.
For diet, food that contains polyunsaturated fats and omega-3, will help build the heart’s health and reduce the risk of heart disease. Such foods include oily fish, vegetables, and fruits. Cutting down on processed food, sugar, saturated fat, and salt will also help.
In terms of medication and other medical interventions, the most appropriate treatment option for a patient will depend on the specific form of heart disease. Generally speaking, some options include medication that will reduce low-density lipoprotein cholesterol, improve blood flow, or reintroduce regularity to the heart rhythm. Surgery, like coronary artery bypass grafting or valve repair or replacement surgery, will also help.
Lifestyle counseling is a form of cardiac rehabilitation that will provide outpatient and long-term treatment to recover from a heart disease problem. It can also reduce the likelihood of one developing.
ACE Inhibitors
There are many medications that can be prescribed to give patients effective treatment for their heart disease.
Angiotensin-converting enzyme inhibitors (ACE) prevent the body from producing angiotensin, a hormone that causes blood vessels to narrow, thereby increasing blood pressure. A medication that inhibits the production of angiotensin will widen blood vessels and let the blood flow more easily, reducing blood pressure and helping the heart beat normally.
ACE inhibitors are normally prescribed for patients with high blood pressure or those who have had heart failure or a heart attack (brought about by some form of heart disease).
Similarly, angiotensin 2 receptor blockers (ARBs) block the angiotensin hormone from working on the heart, also lowering blood pressure.
Anticoagulants and Clotting Factors
Anticoagulants are also used in the treatment of heart disease. Plaque is one of the main contributors to heart disease.
Plaque can cause blood clots, which can be very dangerous when the clot breaks free of the plaque and gets lodged in a heart vessel. This causes a heart attack by blocking blood flow to the heart. The blood clot can also travel to the lungs (where it can cause a pulmonary embolism) or the brain (where it can cause a stroke).
With anticoagulants, blood clots are stopped because the medication prevents the body from producing the right proteins (clotting factors) to create blood clots. Other anticoagulants prevent other chemicals from helping the clotting proteins to form. Anticoagulants cannot break up existing blood clots.
Antiplatelet Drugs and Beta-blockers
Antiplatelet medications also prevent blood clots, but they do so via a different method than anticoagulants. They prevent the body from producing thromboxane, which would normally direct platelets (tiny blood cells that are designed to help the body form clots to stop bleeding) to come together to form a blood clot.
Antiplatelet agents are prescribed for people who have a buildup of plaque in their arteries or those who have an irregular heart rhythm, which can raise the risk of blood clots.
Beta blockers are a wide category of medications that are used to treat different problems from different forms of heart disease. They work by blocking the effects of certain hormones and neurotransmitters that stimulate the heart, like adrenaline (epinephrine). This blocking moves the heart to beat slower and with less force.
A person at risk for heart disease may be prescribed a beta blocker to prevent a first heart attack as well as heart attacks in the future. Patients with irregular heartbeats, chest pain, high blood pressure, or a risk or history of heart failure might also receive beta blockers.
Calcium Channel Blockers and Cholesterol Medications
All the muscles in the body need calcium to work, and the heart is no exception. Patients with certain heart problems might receive calcium channel blockers, which work by controlling the amount of calcium that enters the muscle cells in the heart and blood vessels. As a result, the heart beats a little easier.
Patients with high blood pressure, irregular heartbeats, and chest pains will likely receive calcium channel blockers.
High cholesterol levels in the blood are one of the biggest drivers for plaque buildup. More plaque means smaller blood vessels or even blood vessels that are completely blocked, leading to stroke, heart attack, and many other serious health problems.
Certain medications will lower the “bad” cholesterol levels (cholesterol with low-density lipoproteins), while boosting the “good” cholesterol (cholesterol with high-density lipoproteins). Doing so lowers the risk of dangerous plaque buildup, and this can significantly reduce the chances of death from heart disease.
Digitalis and Nitrate Drugs
For people with weak hearts, digitalis medication increases the amount of calcium cells in their hearts, making the heart pump harder and sending out more blood per beat. The medication also slows down specific electrical signals within the heart. This has the effect of reducing the total electrical activity in the heart, which is useful for people with irregular heartbeats.
Digitalism medications are usually prescribed in combination with ACE inhibitors.
Lastly, nitrate medications work by opening up the blood vessels wider, so blood can pass through the vessels easier. Nitrates will be prescribed for patients with angina (chest pain) or those who have had heart failure in the past or are at risk for heart failure.
A Customized Solution
Finding effective treatments for heart disease can seem difficult because there are so many forms of the condition, with different risk factors, symptoms, outcomes, and remedies. For this reason, it is vital that you check with your doctor if you have any of the risk factors, especially as you age and if you have a family history of heart issues. If you’ve noticed changes or problems with your heartbeat, breathing, stamina, or diabetes, consult your doctor immediately.
The sooner the likelihood of heart disease can be determined, the sooner you can get started on a treatment plan that is right for you.
References
Heart Disease. (March 2018). Mayo Clinic.
Causes and Risks of Heart Disease. (February 2018). Healthline.
The Link Between Smoking and Atherosclerosis. (July 2019). Verywell Health.
Cholesterol and Artery Plaque Buildup. (July 2018). Web MD.
What Are the Symptoms of Heart Disease in Men? (July 2018). Medical News Today.
An Overview of Cardiac Arrhythmias. (June 2019). Verywell Health.
Congenital Heart Disease in Adults. (October 2018). Mayo Clinic.
Dilated Cardiomyopathy. (March 2018). Mayo Clinic.
Endocarditis. (January 2018). Healthline.
Valvular Heart Disease. Johns Hopkins Medicine.
What to Know About Cardiovascular Disease? (July 2019). Medical News Today.
Health Risks of Being Overweight. (February 2015). National Institute of Diabetes and Digestive and Kidney Diseases.
American Heart Association Recommendations for Physical Activity in Adults and Kids. (April 2018). American Heart Association.
Drugs to Treat Heart Disease. (January 2017). Healthline.
ACE Inhibitors and Heart Disease. (September 2018). WebMD.
Anticoagulation in Heart Disease. (1999). BMJ.
Hemophilia, Coagulation, and Blood Clotting. (November 2018). Medical News Today.
Heart Disease and Antiplatelet Drugs. (March 2019). WebMD.
Beta-Blockers for Heart Disease. (January 2018). Healthline.
Heart Disease and Calcium Channel Blocker Drugs. (February 2018). Web MD.
Understanding Cholesterol Numbers. (July 2018). WebMD.
Cholesterol-Lowering Drugs. (March 2016). Healthline.
Treating Heart Disease With Digoxin. (April 2018). WebMD.
Take Nitroglycerin to Ease-and Avoid-a Common Heart Disease Symptom. (March 2014). Harvard Health Publishing.